Muscle Loss Linked to Kidney Risk: New Insights for Chronic Kidney Disease
핵심 흐름 미리보기
- The Silent Connection: Muscle Loss and Kidney Health – What the Latest Research Tells Us
- The link between muscle mass and overall health is becoming increasingly clear. But recent...
- The Growing Concern: CKD Prevalence and the Hidden Impact of Muscle Decline
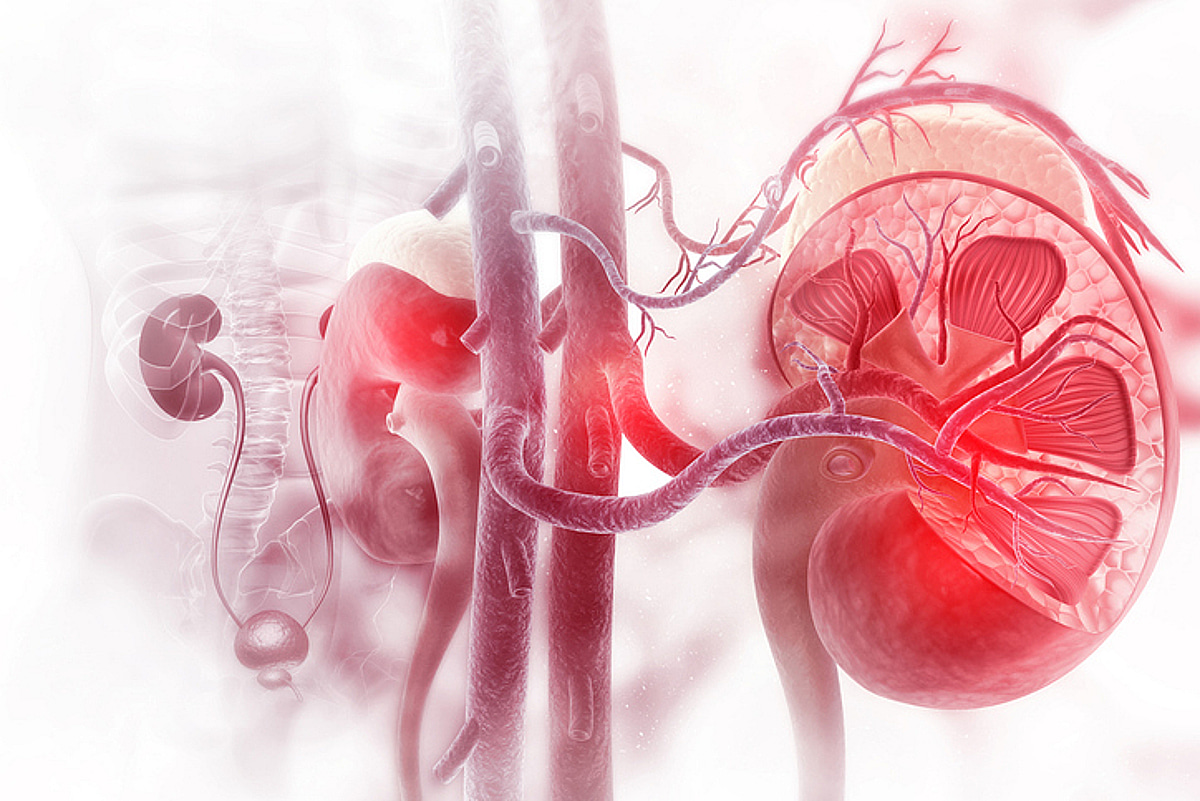
The Silent Connection: Muscle Loss and Kidney Health – What the Latest Research Tells Us
The link between muscle mass and overall health is becoming increasingly clear. But recent research, analyzed as of March 2026, highlights a particularly concerning connection: the relationship between muscle loss (sarcopenia) and chronic kidney disease (CKD). A large-scale analysis, the first of its kind, is shedding light on how the decline in muscle mass and associated nutritional depletion significantly impacts individuals already battling CKD. This isn’t just about aesthetics or strength; it’s about kidney function and overall survival. This post will delve into the findings, explain *why* this connection exists, and offer practical steps – particularly relevant for those living in or visiting Korea – to mitigate the risks. Keywords: chronic kidney disease, sarcopenia, muscle loss, nutrition, kidney health.

The Growing Concern: CKD Prevalence and the Hidden Impact of Muscle Decline
Chronic Kidney Disease isn’t a single disease, but rather a progressive loss of kidney function. Globally, and increasingly in Korea with its aging population, the prevalence of CKD is rising. Many people remain undiagnosed in the early stages, making preventative measures crucial. Traditionally, focus has been on managing blood pressure, blood sugar, and protein intake. However, this new research emphasizes a previously underestimated factor: muscle mass.

The analysis, covering a substantial cohort of CKD patients, revealed a strong correlation between lower muscle mass and faster disease progression, increased hospitalization rates, and a higher risk of mortality. It’s not simply that people with CKD *tend* to lose muscle; the muscle loss itself appears to *accelerate* the decline in kidney function. This is a critical shift in understanding.
Why Does Muscle Matter to Your Kidneys? The Biochemical Link
The connection isn’t coincidental. Several key mechanisms explain why muscle loss negatively impacts kidney health. Firstly, muscle tissue is a major consumer of glucose. When muscle mass decreases, glucose metabolism is impaired, leading to insulin resistance. Insulin resistance, in turn, exacerbates kidney damage.
Secondly, muscle breakdown releases inflammatory markers into the bloodstream. Chronic inflammation is a known driver of CKD progression. The kidneys are particularly vulnerable to inflammatory damage.
Thirdly, and perhaps most importantly, muscle tissue plays a vital role in protein metabolism. CKD patients often struggle with protein-energy wasting (PEW), a condition characterized by both muscle loss and malnutrition. The kidneys are responsible for filtering waste products from protein metabolism. When muscle breakdown increases, the kidneys are forced to work harder, accelerating their decline. This is especially relevant considering the Korean diet, which traditionally includes significant protein intake.
Nutritional Depletion: A Vicious Cycle in CKD
The research highlighted a significant overlap between muscle loss and nutritional deficiencies in CKD patients. This isn’t just about a lack of protein, although that’s a major component. Deficiencies in Vitamin D, essential amino acids, and key minerals like potassium and magnesium were also frequently observed.
These deficiencies contribute to further muscle breakdown, creating a vicious cycle. CKD itself can impair nutrient absorption, and dietary restrictions often imposed on CKD patients (particularly regarding potassium and phosphorus) can inadvertently lead to other deficiencies. For visitors to Korea, understanding the ingredients in traditional dishes is crucial. Many Korean meals are rich in sodium and potassium, requiring careful consideration for those with kidney issues.
Actionable Steps: Building and Maintaining Muscle with Kidney Health in Mind (Especially in Korea)
So, what can be done? Here are three actionable steps, tailored with the Korean context in mind:
1. Prioritize Resistance Training (with Medical Clearance): This isn’t about becoming a bodybuilder. Even moderate resistance training – using weights, resistance bands, or even bodyweight exercises – can significantly slow muscle loss. *Condition:* Obtain clearance from your nephrologist before starting any new exercise program. For those in Korea, many *fitness centers* (헬스장 – helseujang) offer introductory sessions and can tailor programs to individual needs. Look for trainers experienced in working with individuals with chronic conditions.
2. Optimize Protein Intake (Under Medical Supervision): The traditional advice to severely restrict protein for CKD patients is being re-evaluated. While excessive protein can strain the kidneys, *adequate* protein intake is essential for maintaining muscle mass. *Condition:* Work with a registered dietitian specializing in renal nutrition to determine the appropriate protein intake for your stage of CKD and individual needs. In Korea, many hospitals offer dedicated renal dietitians. Be mindful of portion sizes when enjoying Korean BBQ (고기 – gogi) or other protein-rich dishes.
3. Focus on Micronutrient Optimization (Through Diet and Supplementation – with Guidance): Address potential deficiencies in Vitamin D, essential amino acids, and key minerals. *Condition:* Get regular blood tests to identify specific deficiencies and discuss appropriate supplementation with your doctor. While Korean cuisine offers a variety of vegetables, ensuring adequate Vitamin D intake can be challenging, especially during the winter months. Consider fortified foods or supplementation as recommended by your healthcare provider.
Navigating Korean Cuisine with Kidney Disease: A Practical Guide
Korean food is delicious and diverse, but it can present challenges for individuals with CKD. Many dishes are high in sodium, potassium, and phosphorus. Here are a few tips:
* Soups & Stews (국 – guk, 찌개 – jjigae): These are often high in sodium. Request that they be made with less salt (소금 적게 – sogeum jeoge) or ask for a separate bowl of broth to control your intake.
* Kimchi (김치): A staple of Korean cuisine, kimchi is high in sodium and can be high in potassium depending on the ingredients. Consume in moderation.
* Banchan (반찬 – side dishes): Be mindful of pickled vegetables (장아찌 – jangajji), which are often high in sodium.
* Grilled Meats (고기 – gogi): A good source of protein, but be mindful of portion sizes and avoid excessive marinades, which can be high in sodium.
Interpreting the Findings: A Paradigm Shift in CKD Management
This large-scale analysis represents a significant step forward in our understanding of CKD. It moves beyond simply treating the symptoms of kidney disease to addressing the underlying factors that contribute to its progression. The focus on muscle health and nutritional status is a crucial addition to the traditional management strategies.
The implications are clear: early detection of muscle loss, proactive interventions to maintain muscle mass, and personalized nutritional support are essential for improving outcomes for individuals with CKD. This research underscores the importance of a holistic approach to kidney health, recognizing the interconnectedness of muscle, nutrition, and kidney function.
Summary:
Recent research (March 2026 data) demonstrates a strong link between muscle loss and the progression of chronic kidney disease. This connection is driven by metabolic and inflammatory pathways, exacerbated by nutritional deficiencies. Proactive interventions focusing on resistance training, optimized protein intake, and micronutrient management – tailored to individual needs and dietary considerations (especially within the Korean culinary landscape) – are crucial for mitigating risk and improving patient outcomes.
함께 읽으면 좋은 글
이미지 출처
- 출처: Google 이미지 검색(크롤링) | 원문: https://www.mt.co.kr/amp/thebio/2026/03/12/2026031117054628128 | 이미지: https://thumb.mt.co.kr/cdn-cgi/image/w=1200,h=801,fit=cover,bg=whilte,f=auto,quality=high,sharpen=2,g=face/21/2026/03/2026031117054628128_1.jpg
- 출처: Wikimedia Commons | 라이선스: Public domain | 원문: https://commons.wikimedia.org/wiki/File:Desinsertion_du_muscle_CO.jpg
- 출처: Google 이미지 검색(크롤링) | 원문: https://m.health.chosun.com/svc/news_view.html?contid=2026031202194 | 이미지: https://m.health.chosun.com/site/data/img_dir/2026/03/12/2026031202188_0.jpg
'일상' 카테고리의 다른 글
| 여자축구, 4연속 월드컵 진출에도 1승의 한계…우즈벡과의 아시안컵 8강전, 새로운 도약의 기회인가 (0) | 2026.03.13 |
|---|---|
| 심인성 쇼크 생존자, 퇴원 후엔 ‘정신건강’ 관리 관건: 이슈를 숫자로 보면 달라지는 해석 (0) | 2026.03.13 |
| 한은, 중동 리스크 "러우전쟁 당시보다 물가·기대인플레 안정적" 이슈 배경과 다음 흐름 (0) | 2026.03.12 |
| 美 소비자물가 안정에도 '불안'…중동 전쟁이 '최대 변수 (1) | 2026.03.12 |
| 세계 1차대전 정리 (0) | 2026.03.12 |



